The Significance of Staff Training in Memory Care Homes
Business Name: BeeHive Homes of Floydada TX
Address: 1230 S Ralls Hwy, Floydada, TX 79235
Phone: (806) 452-5883
BeeHive Homes of Floydada TX
Beehive Homes assisted living care is ideal for those who value their independence but require help with some of the activities of daily living. Residents enjoy 24-hour support, private bedrooms with baths, medication monitoring, home-cooked meals, housekeeping and laundry services, social activities and outings, and daily physical and mental exercise opportunities. Beehive Homes memory care services accommodates the growing number of seniors affected by memory loss and dementia. Beehive Homes offers respite (short-term) care for your loved one should the need arise. Whether help is needed after a surgery or illness, for vacation coverage, or just a break from the routine, respite care provides you peace of mind for any length of stay.
View on Google Maps
1230 S Ralls Hwy, Floydada, TX 79235
Business Hours
- Monday thru Sunday: 9:00am to 5:00pm
Follow Us:
- Facebook: https://www.facebook.com/BeeHiveHomesFloydada
-
Youtube: https://www.youtube.com/@WelcomeHomeBeeHiveHomes
🤖 Explore this content with AI:
💬 ChatGPT 🔍 Perplexity 🤖 Claude 🔮 Google AI Mode 🐦 Grok
Families hardly ever reach a memory care home under calm circumstances. A parent has begun roaming at night, a spouse is avoiding meals, or a precious grandparent no longer recognizes the street where they lived for 40 years. In those minutes, architecture and features matter less than the people who appear at the door. Staff training is not an HR box to tick, it is the spinal column of safe, dignified take care of locals coping with Alzheimer's illness and other forms of dementia. Trained teams prevent damage, minimize distress, and develop small, regular pleasures that add up to a better life.
I have walked into memory care neighborhoods where the tone was set by peaceful skills: a nurse bent at eye level to describe an unknown noise from the laundry room, a caretaker rerouted an increasing argument with a photo album and a cup of tea, the cook emerged from the kitchen to describe lunch in sensory terms a resident could acquire. None of that occurs by accident. It is the result of training that deals with memory loss as a condition requiring specialized abilities, not simply a softer voice and a locked door.
What "training" actually implies in memory care
The phrase can sound abstract. In practice, the curriculum needs to specify to the cognitive and behavioral modifications that feature dementia, tailored to a home's resident population, and enhanced daily. Strong programs integrate knowledge, method, and self-awareness:
Knowledge anchors practice. New staff learn how various dementias progress, why a resident with Lewy body might experience visual misperceptions, and how pain, irregularity, or infection can appear as agitation. They discover what short-term memory loss does to time, and why "No, you informed me that currently" can land like humiliation.
Technique turns knowledge into action. Employee discover how to approach from the front, use a resident's preferred name, and keep eye contact without looking. They practice recognition treatment, reminiscence prompts, and cueing methods for dressing or eating. They establish a calm body position and a backup plan for personal care if the first attempt stops working. Method also consists of nonverbal abilities: tone, rate, posture, and the power of a smile that reaches the eyes.
Self-awareness prevents empathy from curdling into frustration. Training helps personnel recognize their own tension signals and teaches de-escalation, not only for homeowners however for themselves. It covers boundaries, grief processing after a resident dies, and how to reset after a challenging shift.
Without all three, you get fragile care. With them, you get a team that adjusts in genuine time and preserves personhood.
Safety starts with predictability
The most instant benefit of training is fewer crises. Falls, elopement, medication mistakes, and goal events are all prone to avoidance when staff follow constant regimens and understand what early warning signs look like. For example, a resident who begins "furniture-walking" along countertops might be signifying a change in balance weeks before a fall. An experienced caretaker notifications, informs the nurse, and the group adjusts shoes, lighting, and exercise. No one praises since nothing significant happens, and that is the point.
Predictability decreases distress. People dealing with dementia depend on hints in the environment to understand each minute. When staff greet them consistently, utilize the exact same expressions at bath time, and offer choices in the same format, citizens feel steadier. That steadiness appears as much better sleep, more total meals, and fewer fights. It also appears in personnel spirits. Mayhem burns individuals out. Training that produces predictable shifts keeps turnover down, which itself strengthens resident wellbeing.
The human skills that change everything
Technical competencies matter, but the most transformative training digs into interaction. Two examples highlight the difference.
A resident insists she must delegate "pick up the children," although her children remain in their sixties. An actual action, "Your kids are grown," intensifies fear. Training teaches recognition and redirection: "You're a dedicated mom. Tell me about their after-school routines." After a couple of minutes of storytelling, staff can offer a job, "Would you help me set the table for their snack?" Function returns because the feeling was honored.
Another resident withstands showers. Well-meaning staff schedule baths on the exact same days and try to coax him with a promise of cookies later. He still declines. A skilled team expands the lens. Is the bathroom brilliant and echoing? Does the water feel like stinging needles on thin skin? Could modesty be the genuine barrier? They adjust the environment, utilize a warm washcloth to begin at the hands, use a robe instead of full undressing, and switch on soft music he associates with relaxation. Success looks mundane: a finished wash without raised voices. That is dignified care.
These approaches are teachable, but they do not stick without practice. The best programs include role play. Enjoying a colleague demonstrate a kneel-and-pause approach to a resident who clenches throughout toothbrushing makes the technique genuine. Training that acts on real episodes from last week cements habits.
Training for medical intricacy without turning the home into a hospital
Memory care sits at a difficult crossroads. Numerous residents deal with diabetes, heart problem, and movement impairments alongside cognitive changes. Staff needs to identify when a behavioral shift might be a medical issue. Agitation can be unattended pain or a urinary tract infection, not "sundowning." Hunger dips can be depression, oral thrush, or a dentures problem. Training in baseline assessment and escalation procedures prevents both overreaction and neglect.
Good programs teach unlicensed caregivers to record and communicate observations clearly. "She's off" is less valuable than "She woke two times, consumed half her typical breakfast, and recoiled when turning." Nurses and medication technicians require continuing education on drug side effects in older grownups. Anticholinergics, for example, can intensify confusion and irregularity. A home that trains its group to ask about medication changes when habits shifts is a home that avoids unneeded psychotropic use.

All of this needs to remain person-first. Residents did stagnate to a medical facility. Training stresses comfort, rhythm, and significant activity even while managing complex care. Staff learn how to tuck a blood pressure look into a familiar social minute, not disrupt a cherished puzzle routine with a respite care beehivehomes.com cuff and a command.
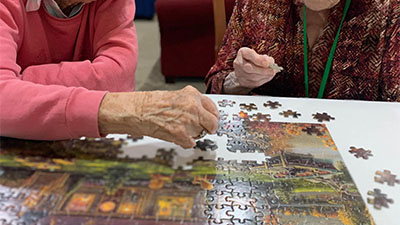
Cultural competency and the biographies that make care work
Memory loss strips away brand-new knowing. What remains is biography. The most elegant training programs weave identity into daily care. A resident who ran a hardware store might react to tasks framed as "assisting us fix something." A previous choir director may come alive when personnel speak in pace and clean the dining table in a two-step pattern to a humming tune. Food preferences carry deep roots: rice at lunch may feel right to somebody raised in a home where rice signified the heart of a meal, while sandwiches sign up as treats only.
Cultural competency training exceeds holiday calendars. It includes pronunciation practice for names, awareness of hair and skin care traditions, and sensitivity to religious rhythms. It teaches personnel to ask open concerns, then carry forward what they find out into care plans. The distinction shows up in micro-moments: the caretaker who understands to offer a headscarf option, the nurse who schedules quiet time before night prayers, the activities director who prevents infantilizing crafts and instead creates adult worktables for purposeful sorting or assembling jobs that match past roles.
Family partnership as an ability, not an afterthought
Families get here with grief, hope, and a stack of worries. Personnel need training in how to partner without handling guilt that does not come from them. The household is the memory historian and should be dealt with as such. Intake ought to include storytelling, not simply kinds. What did mornings look like before the move? What words did Dad use when irritated? Who were the next-door neighbors he saw daily for decades?
Ongoing interaction needs structure. A quick call when a new music playlist triggers engagement matters. So does a transparent description when an incident occurs. Households are most likely to rely on a home that says, "We saw increased uneasyness after dinner over 2 nights. We adjusted lighting and included a short corridor walk. Tonight was calmer. We will keep monitoring," than a home that just calls with a care strategy change.
Training likewise covers boundaries. Families may ask for round-the-clock individually care within rates that do not support it, or push personnel to enforce regimens that no longer fit their loved one's abilities. Knowledgeable staff validate the love and set practical expectations, providing options that protect safety and dignity.
The overlap with assisted living and respite care
Many families move first into assisted living and later to specialized memory care as needs evolve. Residences that cross-train staff across these settings offer smoother shifts. Assisted living caregivers trained in dementia interaction can support homeowners in earlier stages without unneeded limitations, and they can determine when a transfer to a more safe environment becomes proper. Similarly, memory care personnel who comprehend the assisted living model can assist households weigh choices for couples who wish to stay together when only one partner needs a secured unit.
Respite care is a lifeline for household caretakers. Short stays work just when the staff can quickly learn a new resident's rhythms and integrate them into the home without disruption. Training for respite admissions highlights quick rapport-building, sped up safety assessments, and versatile activity planning. A two-week stay must not feel like a holding pattern. With the right preparation, respite ends up being a restorative duration for the resident in addition to the household, and sometimes a trial run that informs future senior living choices.
Hiring for teachability, then building competency
No training program can conquer a poor hiring match. Memory care calls for people who can check out a room, forgive rapidly, and discover humor without ridicule. Throughout recruitment, useful screens aid: a brief situation role play, a question about a time the candidate altered their technique when something did not work, a shift shadow where the individual can sense the pace and emotional load.
Once worked with, the arc of training must be deliberate. Orientation typically consists of 8 to forty hours of dementia-specific content, depending upon state policies and the home's requirements. Shadowing an experienced caretaker turns concepts into muscle memory. Within the first 90 days, staff ought to demonstrate proficiency in individual care, cueing, de-escalation, infection control, and documents. Nurses and medication assistants require added depth in evaluation and pharmacology in older adults.
Annual refreshers avoid drift. People forget abilities they do not use daily, and brand-new research study shows up. Short monthly in-services work much better than infrequent marathons. Turn topics: recognizing delirium, handling irregularity without excessive using laxatives, inclusive activity preparation for men who prevent crafts, respectful intimacy and authorization, grief processing after a resident's death.
Measuring what matters
Quality in memory care can be determined by numbers and by feel. Both matter. Metrics may consist of falls per 1,000 resident days, major injury rates, psychotropic medication frequency, hospitalization rates, personnel turnover, and infection occurrence. Training typically moves these numbers in the best direction within a quarter or two.
The feel is just as vital. Walk a corridor at 7 p.m. Are voices low? Do personnel welcome citizens by name, or shout directions from doorways? Does the activity board reflect today's date and real occasions, or is it a laminated artifact? Residents' faces tell stories, as do households' body movement during gos to. A financial investment in staff training ought to make the home feel calmer, kinder, and more purposeful.
When training avoids tragedy
Two brief stories from practice highlight the stakes. In one neighborhood, a resident with vascular dementia started pacing near the exit in the late afternoon, yanking the door. Early on, staff scolded and guided him away, only for him to return minutes later on, agitated. After a refresher on unmet needs assessment and purposeful engagement, the team learned he utilized to inspect the back door of his store every evening. They offered him a key ring and a "closing list" on a clipboard. At 5 p.m., a caretaker strolled the building with him to "secure." Exit-seeking stopped. A roaming threat ended up being a role.
In another home, an untrained short-term employee tried to rush a resident through a toileting routine, resulting in a fall and a hip fracture. The occurrence unleashed examinations, suits, and months of pain for the resident and guilt for the group. The neighborhood revamped its float pool orientation and included a five-minute pre-shift huddle with a "warning" review of homeowners who require two-person assists or who resist care. The cost of those added minutes was trivial compared to the human and monetary costs of preventable injury.
Training is also burnout prevention
Caregivers can love their work and still go home depleted. Memory care requires persistence that gets more difficult to summon on the tenth day of short staffing. Training does not remove the strain, but it offers tools that lower useless effort. When staff understand why a resident withstands, they waste less energy on ineffective techniques. When they can tag in a colleague utilizing a known de-escalation strategy, they do not feel alone.
Organizations need to consist of self-care and teamwork in the formal curriculum. Teach micro-resets in between rooms: a deep breath at the limit, a quick shoulder roll, a glimpse out a window. Normalize peer debriefs after intense episodes. Deal grief groups when a resident dies. Rotate projects to prevent "heavy" pairings every day. Track workload fairness. This is not extravagance; it is threat management. A regulated nerve system makes fewer mistakes and shows more warmth.
The economics of doing it right
It is appealing to see training as an expense center. Salaries rise, margins shrink, and executives try to find budget plan lines to trim. Then the numbers appear somewhere else: overtime from turnover, agency staffing premiums, survey deficiencies, insurance premiums after claims, and the quiet cost of empty rooms when track record slips. Residences that purchase robust training regularly see lower staff turnover and greater tenancy. Families talk, and they can tell when a home's pledges match day-to-day life.
Some rewards are instant. Reduce falls and health center transfers, and households miss out on less workdays sitting in emergency rooms. Less psychotropic medications means fewer side effects and much better engagement. Meals go more efficiently, which reduces waste from untouched trays. Activities that fit homeowners' abilities cause less aimless wandering and fewer disruptive episodes that pull multiple staff far from other jobs. The operating day runs more efficiently because the emotional temperature is lower.
Practical foundation for a strong program
A structured onboarding pathway that sets new hires with a mentor for a minimum of 2 weeks, with measured proficiencies and sign-offs instead of time-based completion.
Monthly micro-trainings of 15 to 30 minutes constructed into shift huddles, focused on one skill at a time: the three-step cueing technique for dressing, recognizing hypoactive delirium, or safe transfers with a gait belt.
Scenario-based drills that practice low-frequency, high-impact events: a missing out on resident, a choking episode, an abrupt aggressive outburst. Consist of post-drill debriefs that ask what felt complicated and what to change.
A resident biography program where every care strategy includes two pages of life history, favorite sensory anchors, and interaction do's and do n'ts, updated quarterly with household input.
Leadership presence on the floor. Nurse leaders and administrators should spend time in direct observation weekly, offering real-time training and modeling the tone they expect.
Each of these elements sounds modest. Together, they cultivate a culture where training is not an annual box to check but an everyday practice.
How this links throughout the senior living spectrum
Memory care does not exist in a silo. It touches independent and assisted living, competent nursing, and home-based elderly care. A resident may begin with at home support, usage respite care after a hospitalization, transfer to assisted living, and ultimately need a protected memory care environment. When providers throughout these settings share a philosophy of training and interaction, shifts are safer. For example, an assisted living neighborhood might welcome families to a month-to-month education night on dementia interaction, which eases pressure at home and prepares them for future choices. A knowledgeable nursing rehabilitation unit can collaborate with a memory care home to line up routines before discharge, decreasing readmissions.
Community partnerships matter too. Local EMS teams take advantage of orientation to the home's design and resident requirements, so emergency situation responses are calmer. Primary care practices that understand the home's training program might feel more comfy changing medications in partnership with on-site nurses, restricting unnecessary expert referrals.
What families ought to ask when examining training
Families examining memory care typically receive magnificently printed sales brochures and polished trips. Dig deeper. Ask how many hours of dementia-specific training caregivers total before working solo. Ask when the last in-service happened and what it covered. Request to see a redacted care plan that consists of biography aspects. Watch a meal and count the seconds an employee waits after asking a question before duplicating it. Ten seconds is a lifetime, and typically where success lives.
Ask about turnover and how the home steps quality. A community that can address with specifics is indicating openness. One that prevents the concerns or offers only marketing language might not have the training backbone you desire. When you hear residents attended to by name and see staff kneel to speak at eye level, when the mood feels unhurried even at shift modification, you are experiencing training in action.
A closing note of respect
Dementia changes the guidelines of discussion, security, and intimacy. It requests caretakers who can improvise with compassion. That improvisation is not magic. It is a discovered art supported by structure. When homes buy personnel training, they invest in the day-to-day experience of people who can no longer promote for themselves in conventional methods. They also honor families who have actually entrusted them with the most tender work there is.
Memory care succeeded looks practically ordinary. Breakfast appears on time. A resident laughs at a familiar joke. Corridors hum with purposeful motion rather than alarms. Common, in this context, is an accomplishment. It is the item of training that respects the intricacy of dementia and the humanity of each person dealing with it. In the more comprehensive landscape of senior care and senior living, that standard should be nonnegotiable.
BeeHive Homes of Floydada TX provides assisted living care
BeeHive Homes of Floydada TX provides memory care services
BeeHive Homes of Floydada TX provides respite care services
BeeHive Homes of Floydada TX supports assistance with bathing and grooming
BeeHive Homes of Floydada TX offers private bedrooms with private bathrooms
BeeHive Homes of Floydada TX provides medication monitoring and documentation
BeeHive Homes of Floydada TX serves dietitian-approved meals
BeeHive Homes of Floydada TX provides housekeeping services
BeeHive Homes of Floydada TX provides laundry services
BeeHive Homes of Floydada TX offers community dining and social engagement activities
BeeHive Homes of Floydada TX features life enrichment activities
BeeHive Homes of Floydada TX supports personal care assistance during meals and daily routines
BeeHive Homes of Floydada TX promotes frequent physical and mental exercise opportunities
BeeHive Homes of Floydada TX provides a home-like residential environment
BeeHive Homes of Floydada TX creates customized care plans as residents’ needs change
BeeHive Homes of Floydada TX assesses individual resident care needs
BeeHive Homes of Floydada TX accepts private pay and long-term care insurance
BeeHive Homes of Floydada TX assists qualified veterans with Aid and Attendance benefits
BeeHive Homes of Floydada TX encourages meaningful resident-to-staff relationships
BeeHive Homes of Floydada TX delivers compassionate, attentive senior care focused on dignity and comfort
BeeHive Homes of Floydada TX has a phone number of (806) 452-5883
BeeHive Homes of Floydada TX has an address of 1230 S Ralls Hwy, Floydada, TX 79235
BeeHive Homes of Floydada TX has a website https://beehivehomes.com/locations/floydada/
BeeHive Homes of Floydada TX has Google Maps listing https://maps.app.goo.gl/VQckTu3ewiBFL32A7
BeeHive Homes of Floydada TX has Facebook page https://www.facebook.com/BeeHiveHomesFloydada
BeeHive Homes of Floydada TX has an Youtube page https://www.youtube.com/@WelcomeHomeBeeHiveHomes
BeeHive Homes of Floydada TX won Top Assisted Living Homes 2025
BeeHive Homes of Floydada TX earned Best Customer Service Award 2024
BeeHive Homes of Floydada TX placed 1st for Senior Living Communities 2025People Also Ask about BeeHive Homes of Floydada TX
What is BeeHive Homes of Floydada TX Living monthly room rate?
==============================================================The rate depends on the level of care that is needed. We do an initial evaluation for each potential resident to determine the level of care needed. The monthly rate is based on this evaluation. There are no hidden costs or fees
Can residents stay in BeeHive Homes until the end of their life?
================================================================Usually yes. There are exceptions, such as when there are safety issues with the resident, or they need 24 hour skilled nursing services
Do we have a nurse on staff?
============================No, but each BeeHive Home has a consulting Nurse available 24 – 7. if nursing services are needed, a doctor can order home health to come into the home
What are BeeHive Homes’ visiting hours?
=======================================Visiting hours are adjusted to accommodate the families and the resident’s needs… just not too early or too late
Do we have couple’s rooms available?
====================================Yes, each home has rooms designed to accommodate couples. Please ask about the availability of these rooms
Where is BeeHive Homes of Floydada TX located?
==============================================BeeHive Homes of Floydada TX is conveniently located at 1230 S Ralls Hwy, Floydada, TX 79235. You can easily find directions on Google Maps or call at (806) 452-5883 Monday through Sunday 9:00am to 5:00pm
How can I contact BeeHive Homes of Floydada TX?
===============================================You can contact BeeHive Homes of Floydada TX by phone at: (806) 452-5883, visit their website at https://beehivehomes.com/locations/floydada/,or connect on social media via Facebook or Youtube
Take a drive to the Floyd County Historical Museum . The Floyd County Historical Museum offers local history exhibits that create an engaging yet comfortable outing for assisted living, memory care, senior care, elderly care, and respite care residents.